California's SB 525 minimum wage mandate goes into effect on June 1, 2024.
See how we are helping hospitals mitigate expected increases in labor cost.
Hospital Performance Improvement
Zephyr is pleased to announce that it is leading a $30M (Annual Revenue/Cost) Financial Improvement Initiative at an independent rural hospital in California.

CONGRATULATIONS
to PROVIDENCE HEALTH and MOTION PICTURE PROVIDERS on their collaboration for primary care and population health services.



Trusted Advisory Services for Hospitals, Medical Groups, and Other Healthcare Organizations
At Zephyr Healthcare Advisors, we believe that you are more than just a client—you're our partner. Together, we will work collaboratively in finding practical solutions for your organizational challenges and needs.




Working Alongside Each Client to Craft Short- & Long-Term Solutions
We are problem solvers above all else. We use our comprehensive knowledge of the rapidly shifting healthcare industry to create data-driven and customized solutions for addressing your issues and achieving your goals.
We take great pride in forging lasting relationships with our clients and supplying them with the tools and strategies they need to thrive.
Healthcare Advisory Services
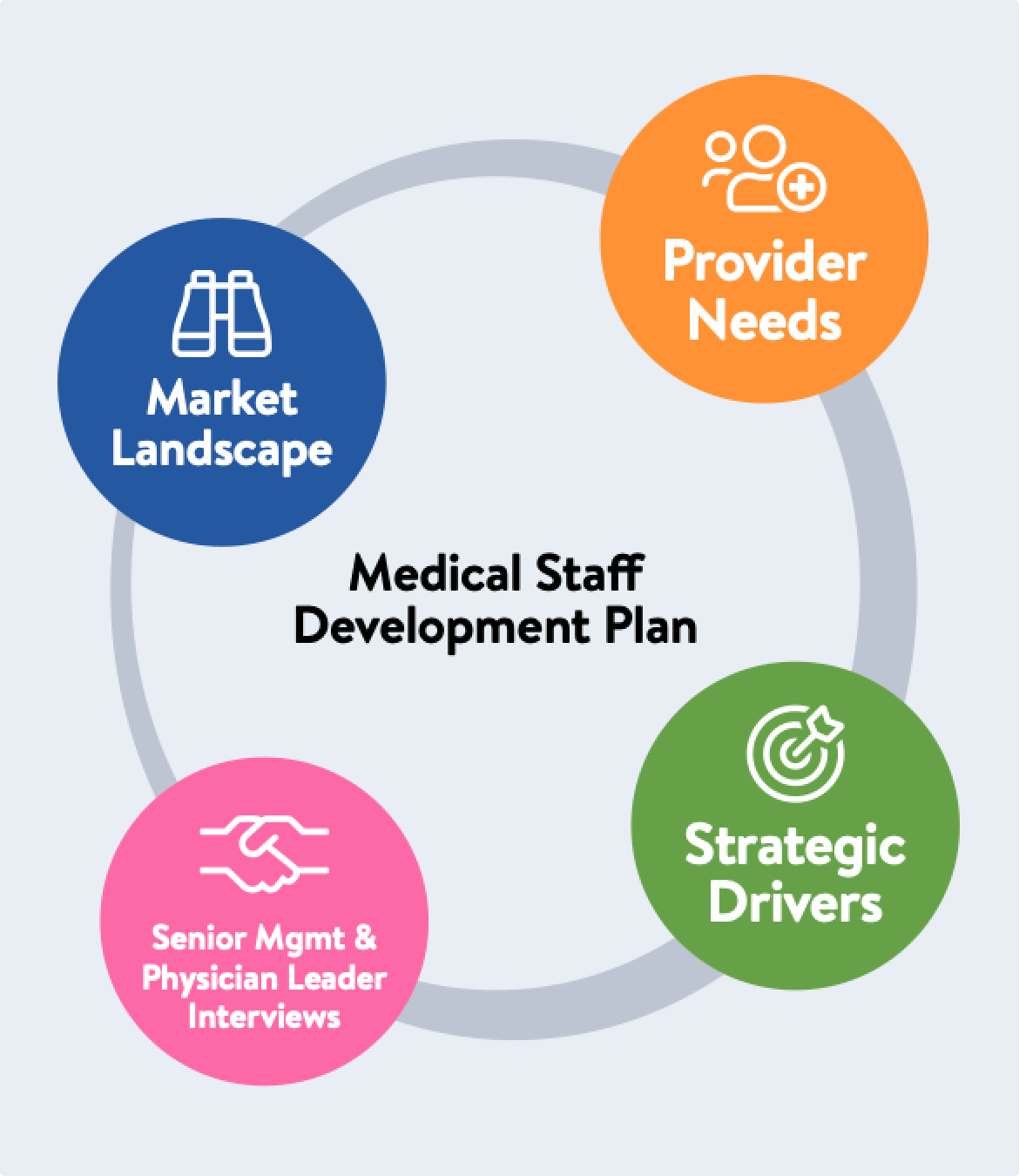
We Partner With You to Develop Data-Driven, Innovative, and Lasting Solutions.
Be a Trusted Advisor
We strive to be a reliable and valuable partner. Our senior team has worked with several client organizations for 10-20 years.
Drive Value
Provide consulting services faster, less expensively and better than industry norms.
Solve Problems
We help identify, vet, and prioritize organizational solutions and assist leaders to solve company problems that keep them up at night.

Creating Innovative and Practical Strategies and Solutions to Help Your Organization Thrive
Our experienced team of healthcare advisors is committed to developing and implementing successful strategies and solutions to support, sustain, and propel our clients forward.
